Sometimes it’s easy as artists to forget we have corporeal bodies with complex operations, and get caught up in the magical world of music. The irony is, with the help of modern science and research, we can figure out how we operate and use that knowledge to optimize our potential – and that’s what this whole website is about!
A major part of the musician’s life is stress. We experience it at our first church Christmas play, relive it, and learn to expect it. We don’t all learn to cope with it – some of us may be genetically inclined to suffer more from it! But physiologically speaking it is a very natural, necessary response our bodies have to perceived threats.


Now what happens when the university student perceives threats every day (from say, deadlines, private lessons, performances, unsolicited smiles from peers…)? The body’s web of communication can get terribly tangled. Couple that constant stress with the the lack of sleep experienced by many students and you have a fairly… bad situation, one from which it can take a long time to recover. This post looks very briefly at some of the physiological components of the stress and sleep systems, and how the performing musician might benefit from a deeper understanding. Or perhaps, just from more (or better) sleep! To start with:
The Brain
The human brain is a ridiculously complex labyrinth of electrical and chemical circuitry (a great starter description can be found here). For the purpose of this blog I’ll focus on certain tidbits of “psychoneuroendocrinology” – how the nervous system interacts with hormones, ideally to maintain a balance.
Neurotransmitters and hormones
The nervous system operates via synapses, where neurotransmitters (chemicals such as amino acids, naturally produced in the body) send messages from one neuron to another. Charged atoms travel from the axon of one neuron to the dendrite of another, hence the “electrical” aspect ascribed to nerves.
Hormones are also chemicals synthesized by the body, but are typically carried by the blood and influence different body cells/tissues. They force a change in the cells they target, hence their name from the Greek hormon: “impel” (Norman et al., 2015).
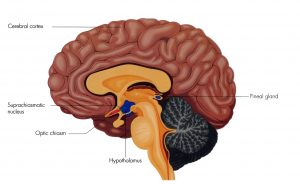
In most situations/functions more than one part of the brain is activated (there is a lot of overlap between sections), but with the stress response we can at least start in the hypothalamus, located towards the centre of the brain (shown in Fig. 1 in blue). It plays a major part in life support including regulating body temperature and monitoring hormones carried by the blood.
HPA-axis
When the brain senses a threat, it “sounds the trumpet” and calls the body to action through the:
– Paraventricular nucleus (PVN found in the hypothalamus) releases cortisol-releasing-hormone (CRH – which stimulates the pituitary gland) as well as vasopressin (a hormone which mainly regulates the body’s water-retention, but may also help regulate other hormones involved in the stress response) (Kalsbeek et al., 2012).
– Pituitary gland releases adrenocorticotropic hormone (ACTH) which in turn stimulates the adrenal glands.
– Adrenal glands release cortisol.
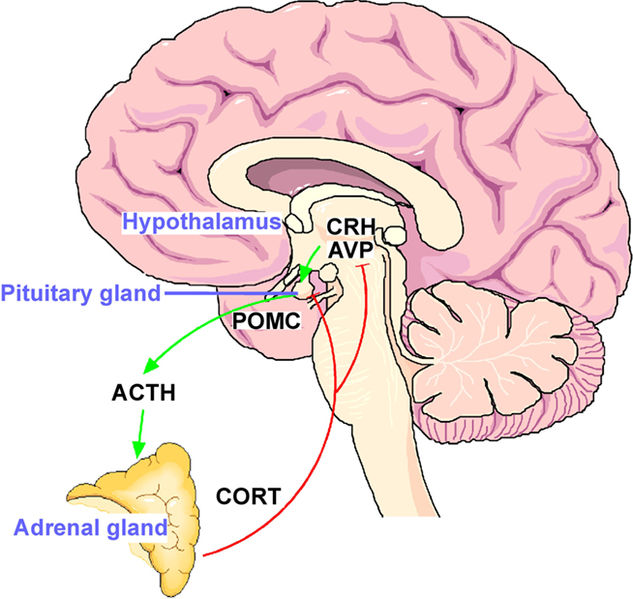
The collective action of the PVN, pituitary, and adrenal glands is referred to as the hypothalamic-pituitary-adrenal (HPA) axis, a model used in most studies on the human body’s stress response.
What does cortisol do? In short, it increases blood sugar (quick energy), suppresses the immune system, and increases metabolism and appetite. If you have some stress-free time, read more about it here! Cortisol works alongside a number of chemicals to keep the body’s systems balanced.
Circadian Rhythms

The hormones involved in the HPA-axis, while essential in response to stress, are also run on a circadian rhythm – derived from “circa”: circle or cycle, and “dia”: day (Nader et al., 2010). Research in the 1940’s already mentions this concept, where organisms’ biological functions are patterned after the 24-hour cycle of the earth’s rotation (Akerstadt, 1978). Many organisms function on such a cycle even in environments lacking the regular change of light/dark (Kalsbeek et al., 2012)!
An essential part of this ~24-hour cycle of a body’s functions is regular rest. Indeed, adult humans spend about a third of every day sleeping. The dark of night has been and is (for the majority of people) time for the body to reset hormone levels, body temperature, etc., and anticipate activity of the next day (Nader et al., 2010).
The Clock: the Suprachiasmatic Nucleus (SCN – also shown in Fig. 1) is considered the “master clock”; here information is received from the eyes, the day is determined, and regular bodily functions are appropriately synced (Kalsbeek et al., 2012). Oxford University is exploring, among other things, how flexible or inflexible the system actually is, and how we as a society might benefit from paying more attention:
A number of studies within the last decade have started connecting the HPA-axis (particularly the end-resulting hormone cortisol) and circadian rhythms – the glands and systems are all set to either circadian (daily) or ultradian (multiple times per day) cycles and hormones are released regularly. Cortisol seems to be secreted approximately once per hour – the differences in concentration are due to varying changes in the amount secreted (Clow et al., 2010).
The science of sleep and the cortisol awakening response
We all sleep, but do we actually understand its characteristics? (I for one, did not!) Copinschi and Challet (2016) describe sleep itself as an ultradian rhythm, a series of approximately 90-minute oscillations of varying brain activity. It can be generally described as non-REM (Rapid Eye Movement) and REM sleep. Non-REM has several stages: it starts lighter (where one may feel like they are falling and jerk back awake) and progressively becomes heavier until one reaches what is also called SWS (Slow Wave Sleep). This is the deepest stage where the brain function is the “quietest” and body functions recover most effectively. After this deep sleep (ranging from nearly an hour long in young adults down to five to ten minutes in older adults) comes the REM when, as one might expect, the eyes move rapidly.
For a fun, slightly more in-depth video on the stages of sleep, try watching Shradda Patel’s video here.
Now a clear example of the HPA-axis’ daily function can be found in the “cortisol awakening response” (CAR), where levels of cortisol seem to increase slightly before one wakes up after the night’s sleep, and rises dramatically in the 20-30 minutes following. This is not solely responsible for, but coincides with the regaining of alertness and appetite (Clow et al., 2010).

How is this useful for the performing musician?
One could compare the body’s hormones as kitchen knives – the more they are used, the less effective they become. Fortunately the human body is a miraculous thing that (generally) self-repairs, and sleep regularly sharpens and resets the systems. But when the stress response is always engaged…
Studies on the cortisol awakening response have indicated that high overall stress (logically) increases overall cortisol levels in the blood and reduces the natural increase prior to and after waking (Clow et al. 2010). Copinschi and Challet (2016) also discuss a reduction in overall cortisol amplitude changes by about 15 per cent, particularly in the absence of sleep.

The performing musician depends (to varying extents) on a functional stress response for an effective performance: heightened alertness, increased energy, slight disillusion that everything will be okay. Cortisol is only one of many substances involved in this, but keeping it in balance helps keep other hormones in balance, and more effective when necessary.
Besides reducing the positive effects, cortisol (and other components of the stress response) have been shown to cause damage if constantly elevated. The hippocampus, a part of the brain especially active in verbal and contextual memory, can be suppressed or “over-loaded” by too much cortisol, so that short-term memory is impaired (McEwen, 1998). Also affected is the immune system involving noradrenaline, where the same effect of over-use (with say, knives) occurs: the regular [quick] response of the system is delayed. So if one catches the “common cold” and should recover within a day or two, the immune system takes longer to respond and may take a week or two! (I can attest to this…)
Another point worth marking is the role age has in the stress response and hormone levels. Levels of cortisol overall increase with age, especially later in the day. This seems to coincide with the system “tiring out” and becoming delayed (such as higher levels of cortisol lasting until late afternoon/evening, when they should be dropping). As it happens, such patterns of longer lasting levels are remarkably similar to those seen in younger adults who are sleep deprived (Copinschi and Challet, 2016)!

So nap!
In an ideal world, we would all get as much sleep as our body needs at night and wake up feeling refreshed every day. Since that does not often happen for the performing (much less studying) musician, we might just find ourselves napping.

Researchers Jaime K. Devine and Jutta M. Wolf decided to explore what a nap actually does to the body’s cortisol levels. Their study was published late 2015 (you can read it here if you’re eager!), and a lot more research can and should be done on the effect of naps on circadian rhythms.
While shorter (30-minute) naps in previous studies had little effect on hormone levels, both the 50-minute and 90-minute naps involved in this study ended with cortisol awakening response; the longer naps seemed to have lower cortisol levels upon waking – more time in sleep suppressing cortisol release – and therefore had a greater increase after waking. This makes sense considering the approximate 90-minute length of the sleep cycle.
Therefore the goal of one’s nap will alter the appropriate time; while a lot of research remains to be done on sleep cycles and just how we might better make use of them, we have a general idea of how long one needs to experience the full cycle under “normal” circumstances. But no research has been done with specific regards to a musician’s hormone levels and perhaps when it would be most effective to nap! Performing on-stage is, in a way, a ridiculous concept for the human body – we expect our brain and our body to maintain peak performance status for one, two, sometimes even three hours. But at the end of a long semester full of stress and off-regular sleep patterns, how is that possible?
I was hoping by the end of this blog to suggest an optimal time for one to nap prior to a musical performance, but the factors involved are too numerous. One must take into account timing adrenaline release, drinking caffeine (if one is inclined) to counter adenosine, lighting which affects the regular cycle of melatonin… the best advice one can take is, in fact, to sleep when you feel tired and wake up when you feel refreshed. On that note, I’d better go to bed.
[toggle title=”On birds:”]Bird brains are indeed different from human brains, but the chemicals involved are surprisingly similar. If one is somehow interested, one may search “bird stress response” or check out this 2005 article on turkeys.[/toggle]
[toggle title=”References”]
Akerstadt, T., Levi, L. (1978). Circadian rhythms in the secretion of cortisol, adrenaline and noradrenaline. European journal of clinical investigation, 8, pp 57-58. http://doi.org.proxy3.library.mcgill.ca/10.1111/j.1365-2362.1978.tb00811.x
Chrousos, G. P. (2009). Stress and disorders of the stress system. Nature reviews endocrinology, 5, pp. 374-381. http://doi.org.proxy3.library.mcgill.ca/10.1038/nrendo.2009.106
Clow, A., Hucklebridge, F., Stalder, T., Evans, P., Thorn, L. (2010). The cortisol awakening response: More than a measure of HPA axis function. Neuroscience and biobehavioral reviews, 35, pp 97-103. http://doi.org.proxy3.library.mcgill.ca/10.1016/j.neubiorev.2009.12.011
Copinschi, G., Challet, E. (2016). Endocrine Rhythms, the Sleep-Wake Cycle, and Biological Clocks. Endocrinology: adult and pediatric (7th ed.), pp. 147-173. http://doi.org.proxy3.library.mcgill.ca/10.1016/B978-0-323-18907-1.00009-3
Devine, J. K., Wolf, J. M. (2015). Determinants of cortisol awakening responses to naps and nighttime sleep. Psychoneuroendocrinology, 63, pp. 128-134. http://doi.org.proxy3.library.mcgill.ca/10.1016/j.psyneuen.2015.09.016
During, H. E., Kawai, M. (2017). The functions of sleep and the effects of sleep deprivation. In Miglis, M. G. (ed.) Sleep and neurologic disease, pp. 55-72. http://doi.org.proxy3.library.mcgill.ca/10.1016/B978-0-12-804074-4.00003-0
Kalsbeek, A., van der Spek, R., Lei, J., Endert, E., Buijs, R.M., Fliers, E. (2012). Circadian rhythms in the hypothalamo–pituitary–adrenal (HPA) axis. Molecular and cellular endocrinology, 349 (1), pp. 20–29. http://doi.org.proxy3.library.mcgill.ca/10.1016/j.mce.2011.06.042
Klein, D. C. (2016). The pineal gland and melatonin. Endocrinology: adult and pediatric (7th ed.), pp. 312-322. http://doi.org.proxy3.library.mcgill.ca/10.1016/B978-0-323-18907-1.00019-6
McEwen, B. S. (1998). Protective and damaging effects of stress mediators. New england journal of medicine, 338, pp. 171-179. http://www.nejm.org.proxy3.library.mcgill.ca/doi/full/10.1056/NEJM199801153380307#t=article
Nader, N., Chrousos, G. P., Kino, T. (2010). Interactions of the circadian CLOCK system and the HPA axis. Trends in endocrinology and metabolism, 21, pp. 277–286. http://doi.org.proxy3.library.mcgill.ca/10.1016/j.tem.2009.12.011
Norman, A. W., Dean, M. C., Henry, H. L. (2015). Hormones (3rd ed.). http://doi.org.proxy3.library.mcgill.ca/10.1016/B978-0-08-091906-5.00001-X
Selye, H. (1950). The general-adaptation-syndrome. Annual review of medicine, 2, pp. 327-342. http://doi.org.proxy3.library.mcgill.ca/10.1146/annurev.me.02.020151.001551[/toggle]
[toggle title=”Media”]
Figures sourced through Creative Commons:
Fig. 1: Suprachiasmatic Nucleus
Fig. 2: HPA-axis
Fig. 3: Earth
Video: “What Makes you Tick: Circadian Rhythms” by OxfordSparks, Creative Commons Attribution license
All other photographs by Jason Biel[/toggle]

Fantastic paper and such useful information! The pictures are an excellent addition to the article.